A paraneoplastic syndrome is a concomitant disease of cancer. However, it is not the result of the tumor, but develops parallel to it. Sometimes the typical symptoms of a paraneoplastic syndrome indicate a malignant tumor that has not yet been discovered and is initially asymptomatic.
What is Paraneoplastic Syndrome?
A paraneoplastic syndrome is always a disease accompanying a malignant tumor. It never develops primarily as a result of neoplasia. Sometimes the symptoms of a paraneoplastic syndrome already appear without the tumor-related symptoms being noticeable. See ezhoushan for What does MLS Stand for.
The typical symptoms of certain paraneoplastic syndromes can often make it easier to diagnose the actual cancer. The symptoms are not a direct result of masses or tissue destruction by the tumor. Rather, they develop as a result of the increased release of certain active substances caused by the tumour.
These can be hormones, antibodies, enzymes or inflammatory factors. The individual clinical pictures present themselves in a correspondingly diverse manner. Paraneoplastic syndromes affect the endocrine system, the skin, the digestive system, the nervous system, the blood or the joints, among others.
Many typical symptoms also occur without an underlying cancer. However, some paraneoplastic syndromes are found exclusively in association with cancer diseases.
Causes
The cause of the paraneoplastic syndrome is the increased formation and release of biologically active substances. There are paraneoplastic syndromes that resemble typical hormone disorders because the tumor produces certain hormones to an increased extent. Endocrine paraneoplastic syndromes are caused, among other things, by neuroendocrine tumors in the pancreas.
These include the so-called insuloma with an overproduction of insulin, the gastrinoma with an increased formation of gastrin, which stimulates gastric acid production, or the Vipom with severe, therapy-resistant diarrhea. Around 20 percent of all tumor patients develop a paraneoplastic syndrome.
Bronchial carcinomas account for the largest proportion at up to 40 percent. In addition to the hormone-related paraneoplastic syndromes, the increased formation of antibodies against cancer cells can also lead to autoimmune-like diseases if these also attack healthy body cells in a cross-reaction.
The prognosis of tumors with antibody-related paraneoplastic syndromes is more favorable than tumors without accompanying symptoms, since the former have a stronger immune reaction against the cancer cells. Some tumors secrete inflammatory factors such as prostaglandins.
Among other things, skin changes, rheumatic complaints or gastrointestinal disorders can occur. Special paraneoplastic syndromes affect the nervous system. Autoantibodies attack nerve cells and cause neurological symptoms.
Furthermore, certain tumors also produce substances that lead to haematological changes. Overall, a large number of different paraneoplastic syndromes can develop.
Symptoms, Ailments & Signs
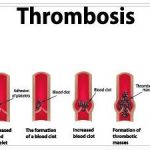
Paraneoplastic syndromes are expressed through general and specific symptoms. Many cancers are accompanied by a general symptom complex of cachexia, increased heat build-up, sweating, thrombosis, leukocytosis, or anemia.
Cachexia manifests itself in constant emaciation, even though enough calories are consumed. This leads to an increased activity of mitochondria in cancer cells, which leads to a very high energy consumption. The metabolism is greatly accelerated, heat generation is increased and fat burning is boosted.
The emaciation in the context of cachexia is therefore not the result of a lack of food, but of increased energy consumption. The specific symptoms include hormone-related disorders. Certain forms of the so-called Cushing’s syndrome occur in bronchial, hepatocellular or renal carcinomas.
The increased release of ACTH stimulates the adrenal cortex to release more cortisol. It comes to a trunk obesity with bull neck and moon face as well as a weakening of the immune system with an increased susceptibility to infections. With an insuloma, too much insulin is produced. The blood sugar level drops dramatically. Other hormones that can be increased in the formation of carcinomas are parathyroid hormone (PTH), vasopressin (ADH), thyrotropin (TSH), calcitonin or serotonin. Calcitonin lowers the calcium level in the blood. Elevated calcium levels are caused by parathyroid hormone.
Increased serotonin concentrations lead to persistent diarrhea and abdominal pain, among other things, because the intestinal peristalsis is constantly stimulated. The TSH in turn stimulates the formation of thyroid hormones in the thyroid gland, causing the typical symptoms of an overactive thyroid gland to appear. Antibody-mediated reactions can lead to autoimmune diseases.
This can lead to rheumatic joint inflammation, inflammatory processes in the gastrointestinal area or neurological deficits. When the skin is involved, the main symptom is excruciating itching. Furthermore, skin lesions, keratoses or increased growth of body hair are observed.
Diagnosis & course of disease
Depending on the complex of symptoms, hormone tests or tests for antibodies can provide information on the cause of certain symptoms. Imaging methods can reveal the underlying tumor.
Complications
In most cases, this syndrome leads to various complications and symptoms, which mainly occur during cancer. The symptoms themselves are very different and can differ greatly from one another. For this reason, no general prediction can be made about the further course of the disease.
Those affected themselves suffer from severe sweating and also from thrombosis. Anemia and thus bleeding or tiredness and exhaustion of the patient also occur. The metabolism of those affected is also affected by this syndrome, so that in most cases the patients also lose weight.
The immune system is significantly weakened by the tumor disease, so that infections or inflammations occur more often, which have a very negative effect on the quality of life of those affected. Itching or lesions on the skin can also occur. Treatment of this syndrome is carried out by treating the tumor. Whether this will be successful cannot be predicted. The life expectancy of the patient may also be reduced by the tumor.
When should you go to the doctor?
Paraneoplastic syndrome only occurs in people who have cancer. Therefore, at the first irregularities and indications of health impairment, a doctor’s visit should be made. Those affected suffer from symptoms such as diarrhea, internal weakness and a general feeling of illness. If you lose weight or start sweating, you should see a doctor. If the affected person suffers from heat build-up, circulatory disorders and general malaise, a doctor’s visit is advisable.
Changes in the complexion, a decrease in physical performance and an increased need for sleep must be examined and treated by a doctor. Disturbances of the digestive tract, rheumatic complaints, an increased susceptibility to infections as well as a repeated fungal infection or an infestation of other germs indicate an illness. A doctor should be informed of the observations and a follow-up visit should be made. Disorders of the hormone system, changes in libido or emotional abnormalities should be discussed with a doctor.
A depressed mood, peculiarities of behavior and changes in personality are to be understood as warning signs of the organism. A doctor’s visit is advisable so that the cause can be investigated. In addition, regular participation in preventive medical check-ups is generally recommended in adulthood. In early detection, the first changes or abnormalities in health can be documented.
Treatment & Therapy
Paraneoplastic syndromes can be treated causally by removing the tumor. This usually goes away with the symptoms. This applies in particular to endocrine-related paraneoplastic syndromes. However, there are also cases where antibody activity remains high after tumor removal.
Of course, the individual tumour-related diseases can be treated separately. Drug therapies or immunosuppression therapies have proven effective in antibody-related paraneoplastic syndromes. Each paraneoplastic syndrome requires its own therapeutic approach. However, if possible, the causal tumor treatment should be sought.
Outlook & Forecast
A paraneoplastic syndrome is not an isolated case, since there are several corresponding syndromes. Doctors regard these as complications of a wide variety of tumor diseases. However, paraneoplastic syndromes are caused neither by the tumor itself nor directly by its metastases. Also, no tumor-related, vascular, metabolic, infectious or treatment-related effects are involved in the development of a paraneoplastic syndrome.
However, a paraneoplastic syndrome can also occur without a recognizable tumor. In this case, it is standard to regularly check for a tumor over a period of two to four years. It has already been proven that the paraneoplastic syndrome occurs in many cases in connection with tumor formation. A distinction must be made between the idiopathic and the real paraneoplastic syndromes.
Even the diagnosis of such syndromes proves to be very complex and difficult. Treatment is also difficult. But it is by no means impossible. Instead of conventional tumor therapy, immunosuppressants are usually used – but only if no tumor could be found. In addition, symptomatic therapies such as pain therapy or other measures are possible.
What is certain is that the type of paraneoplastic syndrome can be used to determine what type of tumor it could be. If this can be discovered early through regular screening and surgically removed, the prognosis improves.
Prevention
There is no general recommendation for the prevention of a paraneoplastic syndrome, as this always accompanies a specific tumor disease. However, the focus of prevention is on the tumors. For example, the risk of developing bronchial cancer can be reduced by leading a healthy lifestyle and not smoking.
Aftercare
Paraneoplastic syndrome is associated with cancer. The effects are not directly attributable to the tumor and are likely due to an immune response or hormonal change. The follow-up care of the paraneoplastic syndrome is therefore connected to the follow-up care of the actual cancer and merges with it.
Depending on the cause, it is not necessarily the case that the paraneoplastic syndrome will go away on its own, even after the tumor has been removed. The body’s reactions persist, especially if the cause of the development of the disease is antibodies that also attack the healthy tissue in the body. In the follow-up care, the specialist, here an oncologist, will take care of the symptoms of the syndrome and treat them at the appropriate check-ups.
Since the symptoms of the paraneoplastic syndrome are diverse, one cannot assume uniform aftercare. The subsidence of the symptoms also varies greatly from person to person and is linked to the causative cancer and accordingly to the trigger of the paraneoplastic syndrome. Whether medication or other aids are required in aftercare cannot be said in general terms. The oncologist can advise patients individually. The follow-up appointments should be adhered to conscientiously.
You can do that yourself
Since the paraneoplastic syndrome is often a parallel disease to a malignant tumor, this tumor must be discovered and treated – if it has not already happened. Otherwise, the paraneoplastic syndrome shows up with different symptoms, which should be approached individually.
A major focus here is diet, as patients can develop life-threatening cachexia. The cancer cells consume so many calories that the patient is no longer able to consume enough nutrients even with a normal diet. There is a tumor-related weight loss. In this case, high-calorie but healthy foods are recommended, such as avocados, bananas or peanut butter as a spread.
The immune system is also weakened by the paraneoplastic syndrome. Patients who want to do something for themselves are therefore advised to do anything that strengthens the immune system: This includes adequate sleep as well as a healthy diet with fresh, high-fiber food, but little sugar and fat. Probiotics, which enrich the intestinal flora, are also recommended. Of course, the patients should not smoke or drink alcohol, so as not to unnecessarily burden the organism. Studies show that exercise can be as important as medication. Even short walks in the fresh air activate the immune system, regulate the metabolism and thus ensure a better quality of life.