Periodontosis, which is often incorrectly referred to as paradontosis in the vernacular, is actually periodontitis. This form of gum disease causes inflammation of the periodontium and the periodontium. This disease is mostly caused by gum inflammation caused by bacteria. If the periodontal disease is not treated, it can lead to tooth loss over time.
What is periodontitis?
Periodontitis or parodontosis is a bacterial inflammation of the periodontium.
If left untreated, it would be destroyed, but the decay process can now be stopped. One form of the disease can start at the root tips, while the other starts at the gum line and extends into the roots. See ezhoushan for What does Kauda Syndrome Stand for.
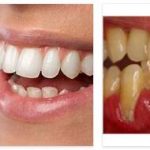
Periodontitis causes sensitive gums and bleeding gums, bad breath and pus formation in the gum area. In advanced periodontitis, the tooth loosens noticeably.
Causes
Periodontitis can only develop if there is sufficient plaque containing bacteria. Tartar can form from this, allowing the bacteria to damage the tooth unhindered. They penetrate into the interior of the teeth and cause inflammation there. The body tries to fight off the bacteria by itself breaking down the tissues in which they exist – in this case, this affects the tooth itself. Therefore, the proof of periodontitis consists in diagnosing the radiographically detectable bone loss.
Among other things, the body produces enzymes to defend itself, which on the one hand are intended to destroy the bacteria, but on the other hand also have harmful effects on the tissue itself. The causes that favor the risk of periodontitis include tobacco use, generally inadequate oral care, unfavorably located piercings and a general weakness of the immune system. Tooth decay also has an increasing effect on the risk of disease – especially when it is open.
Symptoms, Ailments & Signs
Periodontitis (periodontal disease) often goes unnoticed at first. The first signs are only weak and are ignored when brushing your teeth every day. If gums bleed repeatedly, this can be an indication of gum inflammation (gingivitis). These abnormalities can be discovered particularly when biting into an apple.
Gingivitis makes the gums more sensitive to touch and even more susceptible to the spread of bacteria. The inflamed area of the oral cavity could present itself as a precursor to periodontal disease. Brushing your teeth is perceived as painful. Accumulated bacteria cause a strong-smelling halitosis. An unpleasant taste also occurs.
These symptoms intensify if purulent areas develop as the disease develops. As the bacterial inflammation progresses, the gums recede in the area of the periodontium. If the inflammation affects the fibers of the periodontium, so-called periodontal pockets develop. This will facilitate the entry of bacteria. Late signs of periodontitis are regression of inflamed jawbones.
The necks of the teeth are increasingly exposed as the gums and jawbone recede. The teeth react more and more strongly to cold and warm stimuli. In the case of severe, untreated periodontitis, the periodontium ultimately no longer functions. The teeth become loose and misaligned teeth form, which can lead to tooth loss. In the case of a rarely occurring aggressive periodontitis, the acute inflammation of the gums also manifests itself with fever and swelling of the lymph nodes.
course of the disease
Schematic representation of healthy gums, periodontal disease and gingivitis. Click to enlarge.
Periodontosis or periodontitis is usually a chronic, intermittent health condition that develops over a long period of time and is often only noticed years later.
It is mostly painless, the first symptom recognized by the patient himself is the loosening of the teeth. In the first phase of periodontal disease, the bacteria in the plaque can still be fought off to a large extent, they do not penetrate the tooth.
Over time, however, the body’s defense cells die off, as do the bacteria – these are stimuli to which the body reacts. He starts to break down the tooth to take away the living space for the bacteria.
Initially, the gums become red, bleeding and bad breath, the further the bacteria penetrate the tooth. A special form is aggressive periodontitis, which leads to the first symptoms much faster and can already occur in childhood.
Complications
If certain risk factors are present, periodontitis can be difficult and not heal properly despite dental treatment. One of the biggest risk factors is smoking. Those affected who suffer from metabolic disorders such as diabetes mellitus or suffer from a weakened immune system must also expect a more difficult course. An unbalanced diet, especially the regular consumption of sweets, is also considered particularly counterproductive in this case.
Sometimes periodontitis can become chronic and accompany a patient for a lifetime. Due to the chronic inflammation, the gums usually bleed profusely, and gum pockets also form. In the next stage, the gums recede. This makes the teeth look longer, sometimes bigger.
At this stage, those affected often suffer more from the aesthetic impairment than from the disorder itself. However, further complications can be expected as the periodontitis progresses. In the medium term, the inflammation destroys the connective tissue and the bony structures of the jaw. Teeth begin to loosen and eventually fall out.
There is also evidence that untreated or chronic periodontitis can result in serious complications. A statistical connection with respiratory diseases and atherosclerotic vascular diseases such as heart attacks and strokes has been demonstrated.
When should you go to the doctor?
Your teeth should always be checked and cleaned at regular intervals by a doctor. If there are no other disorders, an annual visit to a dentist is recommended. If gum bleeding occurs repeatedly or suddenly despite the checks that have taken place, this indicates an irregularity. A dentist should be consulted so that the cause can be investigated. If you have bad breath, an unusual taste in your mouth, or if you have pus, you need to see a doctor.
Open wounds must be treated sterile, otherwise there is a risk of sepsis. If discrepancies such as bleeding, discomfort or pain start immediately with the daily tooth cleaning, it is advisable to clarify the symptoms. If the gums recede continuously, there is a need for action. Loosening of the teeth or an existing denture should be presented to a doctor.
An examination is recommended as soon as possible, since the symptoms will increase over time. If there are changes in the jawbones or displacements of the jaws, a doctor is needed. If left untreated, there is a risk of tooth loss, which should be prevented in good time. If the person concerned complains of fever or if swelling of the lymph is noticed, a doctor’s visit is recommended. In these cases, the germs and bacteria from the mouth and throat have already spread and trigger sequelae and other diseases.
Treatment & Therapy
The aim of treating periodontal disease is to eliminate the inflammatory factors in the mouth, thereby restoring health over the long term. To do this, the patient’s teeth are first analyzed in detail in order to determine the severity of the disease. Once the bacteria have been identified and systemic disease has been ruled out, all visible evidence above the gumline is removed by the dentist.
Fillings may also have to be made during this phase if cavities have formed in the teeth due to tooth decay. Then the same treatment is carried out with all deposits that lie below the gums in order to free them from bacterial deposits as well. Depending on the severity of the periodontitis, it may be necessary to additionally treat the periodontitis with antibiotics in order to eliminate all bacteria that have accumulated in the tooth in the long term.
Aftercare
Periodontitis follow-up care is very important. The colonization of bacteria that can trigger periodontitis must be consistently prevented even after treatment has been completed. In this respect aftercare is the same as prevention in the essential points.
This applies above all to consistent oral hygiene. But brushing your teeth regularly with the right brushing technique is not enough. There are places that cannot be reached by the toothbrush. This applies in particular to the so-called gum line (the transition between tooth and gum) and the sometimes very fine spaces between the teeth.
Here the PZR (professional tooth cleaning) is the right method for maximum oral hygiene. Hard plaque (tartar) and soft plaque (biofilm) in hard-to-reach places are thoroughly removed. Due to its efficient effect, the PZR is not only reimbursed by many health insurance companies during the aftercare period.
Apart from oral hygiene, there are a number of things to consider in the aftercare of periodontitis. Ideally, smokers think about quitting nicotine. Nicotine has a habit of narrowing the vessels. This means that bleeding gums as an alarm signal of periodontitis may not appear at all or only much later than with other sufferers and valuable time is wasted. Chewing food intensively for optimal salivation is important and can also become a useful routine in aftercare.
Outlook & Forecast
Patients with periodontitis must consult the dentist at regular intervals. The prognosis depends, among other things, on the type and severity of the disease. For example, numerous secondary diseases can develop from a periodontitis apicalis. These include apical cysts, abscesses or granulomas, which can lead to bone or root dissolution. Other forms of the disease can also lead to diseases such as diabetes or rheumatism. Even cardiovascular diseases are not excluded.
However, if periodontitis is detected and treated early, the prognosis is relatively good. The symptoms should have largely disappeared after a few treatments. Late effects are not to be expected with early therapy. However, patients must visit the doctor regularly and should strive for good oral and dental hygiene.
The prognosis is usually made by the dentist or dentist who takes over the treatment. Patients with periodontitis have the prospect of a symptom-free life. It should be noted, however, that long-term effects can occur if the teeth are not properly cared for after the end of the treatment. Life expectancy is not reduced by periodontitis.
You can do that yourself
Eine Parodontitis muss in der Regel zahnmedizinisch behandelt werden. In leichten Fällen oder ergänzend zur schulmedizinischen Therapie kann eine Selbstbehandlung mit Hausmitteln versucht werden: Mundspülungen mit Salbei, Thymian oder einer einprozentigen Wasserstoffperoxid-Lösung wirken ebenso wie Teebaumölantibacterial – they can reduce inflammation and in some cases stop receding gums. Massage of pain-relieving and anti-inflammatory aloe vera gel into the reddened areas several times a day has also proven effective. Clove oil can be used against bleeding gums and aching tooth necks. The effectiveness of green tea has been proven in some studies: According to them, two cups a day can prevent the progression of periodontal disease.
A varied diet with plenty of fresh fruit, vegetables and dairy products provides the body with all the minerals and vitamins necessary for healthy teeth and bones. In addition, the immune system is strengthened, so the body can fight the triggering bacteria more effectively. Proper oral hygiene is also very important: To protect sensitive gums, we recommend using a soft toothbrush, and you should always brush from the gums to the teeth. Brushing your teeth immediately after eating can do more harm than good, especially after consuming acidic drinks or food: a waiting period of at least half an hour is recommended.