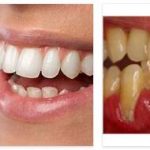
Hailey -Hailey disease is an autosomal dominant skin disease. Individual areas of the patient’s skin blister when exposed to external influences such as UV light. Invasive and drug-based methods are available for treatment.
What is Hailey-Hailey disease?
Blistering of the skin can have a variety of causes. One possible cause is Hailey-Hailey disease. With this skin condition, the skin blisters from birth. The disease is accordingly a congenital skin disease that is counted among the congenital skin malformations. See homethodology for Impulse Control Disorder Overview.
Hailey-Hailey disease was first described in 1939. The first description goes back to the American brothers William and Hugh Hailey, both of whom worked in dermatology. In addition to the term Hailey-Hailey’s disease, different names have now been established for the disease. These include chronic recurrent acantholysis or dyskeratosis bullosa hereditaria, which are synonymous terms for familial benign pemphigus.
But the terms Hailey-Hailey syndrome, Hailey-Hailey disease, Gougerot-Hailey-Hailey disease, recurrent herpetiform dermatitis and pemphigus chronicus benignus familiaris are also used for the clinical picture. The skin disease is a hereditary disease that is sometimes assigned to the superordinate group of dermatoses and immediately catches the eye during visual diagnostics due to typically arranged erosions of the skin.
Causes
The blistering associated with Hailey-Hailey disease is acantholytic in nature. Cells that control corneal formation are normally located in the spinous layer or germ layer of the epidermis, i.e. in the epidermis. In patients with Hailey-Hailey disease, the skin-forming cells detach from the epidermis, causing blisters to form.
The cause lies in a hereditary mutation of the ATP2C1 gene, which codes for an ATPase, i.e. an ATP-splitting enzyme. The mutation results in abnormally structured ATPases. As a result, the Ca content in the Golgi apparatus decreases and faulty processing for adhesion molecules occurs. In addition, cell-to-cell adhesion and adhesions for acantholysis are insufficient.
Hailey-Hailey disease is inherited in an autosomal dominant manner with variable penetrance. In addition to the endogenous causal factors, exogenous influences such as moisture, heat and microbes play a role in the onset of the disease. The endogenous factors alone cause only a genetic disposition.
If the disposition is appropriate, exposure to the exogenous factors leads to the outbreak of the disease. Heavy sweating, infections, heat and UV exposure are important influences in this context.
Symptoms, Ailments & Signs
Patients with Hailey-Hailey’s disease suffer from blistering of the skin, which occurs particularly in the moist, warm armpits and groin area. The skin changes are initially erythema or skin reddening, which occur due to increased blood flow after inflammatory processes. In many patients, the neck and anal area are affected in addition to the armpits and groins.
The skin pigmentation changes in the corresponding areas. The result is discoloration of the skin. In addition to the skin symptoms, most of those affected suffer from severe itching. Apparently there is an increased risk of superinfection. Many case reports describe, for example, recurring infections with bacteria on the inflamed skin.
The skin changes usually appear as weeping areas, which often have a crusted and cracked surface. The severity of the disease can vary from case to case and is essentially related to external factors. The first manifestation of the skin disease does not have to be immediately after birth. Only the disposition is innate.
Diagnosis & course of disease
The family history plays an increased role in the diagnosis of the autosomal dominant inherited Hailey-Hailey disease. Some skin diseases are easily confused with Hailey’s disease Hailey. To establish a diagnosis, a differential diagnostic exclusion of erythrasma, fungal infections of the skin and candida intertrigo is required.
Pemphigus vegetans, a severe and chronic skin disease of unknown cause, should also be ruled out as a possible disease. Molecular genetic detection of the causative mutation can undoubtedly confirm the diagnosis of Hailey-Hailey disease, but is rarely carried out because of the high costs.
Complications
In most cases, Hailey-Hailey disease leads to impairments on the patient’s skin. This mainly leads to the formation of blisters and other unpleasant symptoms on the skin, which can significantly reduce the quality of life of those affected. Furthermore, the skin often turns red and itching occurs.
Inflammation can also occur on the skin and lead to inferiority complexes or reduced self-esteem in those affected. Children can also be bullied or teased by the symptoms of Hailey-Hailey disease. In some cases, the disease leads to hyperpigmentation. The skin itself becomes cracked and infections or inflammation of the skin occur more often.
Unfortunately, Hailey-Hailey’s disease cannot be treated causally. For this reason, treatment is primarily aimed at reducing the symptoms and complaints. There are no further complications. With the help of creams and antibiotics, it is possible to limit the symptoms. The life expectancy of those affected is usually not reduced by Hailey-Hailey disease. In severe cases, surgical interventions are also necessary.
When should you go to the doctor?
Abnormalities and changes in the complexion are signs of an existing irregularity. If blisters form on the skin, a doctor should be consulted. If the blisters multiply when exposed to light, this is to be understood as a characteristic feature of Hailey-Hailey disease. The armpits, neck, anal area or groin area are particularly affected by the changes. Redness or recurring inflammation indicate a disease that needs to be clarified and treated. Changes in pigmentation and itching should be presented to a doctor.
If the itching leads to open wounds, the wound must be treated sterilely, otherwise germs can get into the organism and cause diseases. Since in the worst case there is a risk of blood poisoning with a potential danger to life, the wound care should be taken over by a doctor if the person concerned cannot take care of it to a sufficient extent. Patients with Hailey-Hailey disease are at increased risk of superinfection. Therefore, a doctor should be consulted at the first irregularities in wound healing. Crusting, wet sores, or cracked layers of skin should be presented to a doctor. Although it is a genetic disease, there is a possibility
Treatment & Therapy
There is no causal therapy for patients with Hailey-Hailey disease. Those affected are treated accordingly supportive and symptomatic, but their disease is not curable. One of the most important steps in treatment is education about the exogenous factors. Since not everyone affected reacts strongly to the same factors, the triggers that are particularly risky in individual cases must first be determined.
If the event is happening, these triggers are avoided as far as possible. Some patients also benefit from avoiding any skin contact that could cause additional skin irritation. In the case of an acute illness, the blisters are usually treated locally with glucocorticoids. The drug-based conservative treatment often takes place in combination with the administration of antibiotics.
In the case of a particularly severe course, systemic application takes place. In some cases, invasive therapy is used. This form of treatment usually corresponds to a dermabrasion. The doctor removes the affected skin layers of the epidermis either with the laser or carries out a plastic surgical procedure.
Both invasive treatments have shown long-term improvement in the past. Nevertheless, the severity of the symptoms decides whether the benefit in the individual case outweighs the risks of an operation. In most cases, inpatient admission is not required for laser treatment. In many cases, local anesthesia is used to reduce the risks.
Outlook & Forecast
Hailey-Hailey disease offers a comparatively good prognosis. By avoiding typical triggers, the symptoms can be largely contained. However, if you break out in a sweat, there is a risk of serious complications. Symptoms such as sensitive itching and infections have a negative effect on well-being and should therefore be avoided. Life expectancy is not reduced by Hailey-Hailey disease.
In individual cases, however, serious health complications occur as a result of superinfection. It can lead to blood poisoning, which can be fatal. Cortisone preparations, antibiotics and modern measures such as dermabrasion have also improved the prognosis in recent years. Most sufferers can lead a symptom-free life without major restrictions.
However, a causal treatment of the condition is not yet available, which is why the sufferers are often dependent on comprehensive treatment for the rest of their lives. The responsible dermatologist or an internist makes the final diagnosis. He consults the symptoms and the severity of the disease. If necessary, the course of the disease of sick people from the environment of the sick person is also consulted in order to make the prognosis.
Prevention
Hailey-Hailey’s disease can only be reliably prevented insofar as sick parents want to do without their own children. On the other hand, although their own children are born with a disposition, they do not necessarily have to develop the disease. Since Hailey-Hailey’s disease does not threaten the life of the patient, the decision not to have children is debatable.
Aftercare
Hailey-Hailey’s disease, also known as pemphigus chronicus benignus familiaris, usually has a chronic, relapsing course. The occurrence of symptoms is often triggered by trauma, heat, moisture or the colonization of microorganisms. Therefore, during aftercare, care must be taken to wear appropriate clothing that prevents the above-mentioned, i.e. not chafing or too tight-fitting.
If, in the context of stubborn recurrences, the affected areas are surgically removed, appropriate aftercare of the wound must be ensured. This includes regular dressing changes and removal of any sutures used when the time comes. If a COs laser treatment has taken place as a therapy option, special attention must be paid to appropriate aftercare. The skin will burn about one to two hours after the laser treatment, and a cool pack can be used to cool it down.
There should be no water contact for the first 24 hours. In the three to five days that follow, care should be taken to ensure that the skin is gently moisturized using appropriate, highly effective preparations. Since the newly formed skin is very sensitive, exposure to the sun should be strictly avoided. In the next one to three months, the use of highly moisturizing skin care products is very important. In addition, consistent light protection of at least SPF 25 is recommended.
You can do that yourself
Hailey-Hailey’s disease sometimes leads to irregularities during healing. In this case, it is necessary to consult a doctor to avoid worse consequences. The incrustations, cracked skin or weeping wounds may otherwise lead to new problems. This also applies to any itching that occurs or to changes in the pigmentation of the skin.
It is very important to protect the skin by wearing loose clothing. Clothing that is too tight could irritate the skin. Constant skin contact with other people can also lead to unfavorable consequences. Other risk factors are too much UV radiation and extreme heat. Those affected should therefore avoid situations in which they sweat profusely. The moisture could encourage infections.
In order to promote wound healing, it is worthwhile to observe certain precautionary measures. Sick people react differently to the various factors, so it is important to know your own sensitivity. Some triggers for increased infections are associated with a higher risk and should be avoided accordingly. In any case, the skin should be irritated as little as possible. In addition, patients should always follow the doctor’s recommendations closely and exercise caution in their daily activities.