The postthrombotic syndrome is the result of phlebothrombosis of the deep veins of the arm or leg and corresponds to a reflux congestion with defects in the venous valves. The cause of PTS is the body’s attempt to heal itself, which wants to make the veins permeable again after a thrombosis. Treatment of PTS focuses on compression and movement.
What is postthrombotic syndrome?
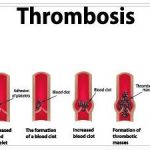
Thrombosis is local intravascular blood clots in the circulatory system. They are usually preceded by changes in the vessel walls, abnormalities in blood flow or changes in blood composition. Phlebothrombosis are special forms of thrombosis, which cause thrombotic occlusion of deep veins and are associated with the risk of pulmonary embolism. See healthknowing for What is the Definition of Health Center.
The deep veins include the deep leg and arm veins. Postthrombotic Syndrome (PTS) summarizes the pathological consequences of permanent damage in the deep vein system of the legs and arms. After an endogenous inflammatory process, the venous valves are often damaged as a result of the closure. A chronic reflux congestion is the result.
The arms are less frequently affected by PTS than the legs. Venous insufficiency can develop from a postthrombotic syndrome after phlebothrombosis. Four stages of PTS are known: stage I with a tendency to edema, stage II with hardening, stage III with sclerotic tissue changes and stage IV with extensive ulcerations.
Causes
PTS is caused by phlebothrombosis of the deep veins of the arm or leg. The closure is usually permanent in nature and lasts for several days. The body tries to dissolve the clot in the vein by initiating an inflammatory process in the vein wall. Only rarely does complete dissolution of the clot actually occur.
The immunologically inflammatory reaction corresponds to an attempt at self-healing, which is intended to make the vital veins permeable again. In the case of inflammation, the venous valves in the affected area are often attacked or destroyed.
The venous valves form an essential part of the reflux mechanism. If they are destroyed, the affected veins are no longer fully functional. It is from this connection that the postthrombotic syndrome develops. Almost half of all patients with thrombosis of the deep arm or leg veins suffer from the phenomenon.
Symptoms, Ailments & Signs
Patients with postthrombotic syndrome suffer from a complex of different symptoms. The main symptom is backflow obstruction in the affected vein. On the basis of this phenomenon, abnormal sensations occur in the respective extremities, such as a feeling of heaviness or tension pain.
As a result of the backlog, edema can form over time. In addition, there are often restricted movements of the affected extremity. Symptoms also appear on the skin of patients as the syndrome progresses. The most common skin symptoms are trophic disorders associated with thinning of the skin epithelium. In addition, pigment changes can occur.
In many cases, wound healing in the affected area is impaired. After the smallest injuries, wound healing disorders can occur, which are often associated with chronic ulceration. Leg ulcers, swelling and pain are associated symptoms of PTS. The severity of PTS depends on the severity of the causative thrombosis and personal factors such as previous illnesses, occupation or gender.
Diagnosis & course of disease
The diagnosis of the postthrombotic syndrome is made using duplex sonography or X-ray examinations using contrast medium. The venous occlusions, including the bypass circuits, are usually clearly visible on the imaging. In individual cases, venous thrombosis is not recognized for several years.
In these cases, a postthrombotic syndrome can develop unnoticed and unforeseen, before the patient even knows about the thrombosis that has occurred. For patients with postthrombotic syndrome, the prognosis depends on the severity and time of diagnosis of the initial thrombosis. The earlier the thrombosis and the subsequent syndrome are detected, the better the prognosis.
Complications
Those affected by this syndrome suffer from various symptoms. As a rule, severe discomfort or sensory disturbances occur in the extremities. This may make the patient’s everyday life more difficult, resulting in significant limitations. In some cases, the syndrome causes those affected to depend on the help of other people in their lives.
Movement restrictions are also not uncommon, so that the patient may need a walking aid. Furthermore, most of those affected suffer from a wound healing disorder. Even minor injuries can lead to severe bleeding or wounds that do not heal. The joints are also often swollen and painful. The syndrome has a very negative effect on the patient’s quality of life and can also lead to psychological problems or depression.
The treatment of this syndrome is usually carried out with the help of medication and compression stockings. There are no complications. Various therapies are also necessary to relieve the symptoms permanently. Life expectancy is usually not reduced or otherwise affected by the syndrome.
When should you go to the doctor?
In the case of sudden or intense disturbances in blood circulation, a doctor is required. If they persist or increase in intensity, they are to be understood as a warning from the organism. There is a need for action, since acute health-threatening conditions can develop in severe cases.
Restrictions in mobility, unsteady gait, dizziness or an inner weakness should be presented to a doctor. If there are changes in the complexion, abnormal sensations on the skin or pain, the affected person needs help. Numbness in the extremities, a tingling sensation on the skin and sensory disturbances are considered uncommon. They should be presented to a doctor as soon as they appear unabated for several days or weeks.
Swelling, the formation of ulcers or edema should be checked out by a doctor. A doctor should be consulted if there is pressure sensitivity, changes in the layers of the skin or a feeling of inner heaviness. Irregularities in the natural healing of wounds, an increased body temperature or a general feeling of illness should be examined and treated.
It is characteristic of the disease that even small wounds show a problematic development. If the person concerned notices a decrease in physical performance, if they tire quickly, if they feel generally unwell or if their resilience is low, medical help should be sought.
Treatment & Therapy
For patients with postthrombotic syndrome, the basic principle of the application of compression is the focus of treatment. Compressions can be applied externally by applying compression bandages or initiated with medical compression stockings. The muscle pump must be activated during compression therapy.
For this reason, the patient has to actively move the affected extremity regularly, for example by cycling or going for walks. The movement units must not overload the affected extremity. Extreme endurance sports should therefore be avoided. In the resting position, the affected extremity is ideally elevated to additionally relieve the damaged venous system.
In individual cases, patients receive diuretic medication. Anticoagulants with inhibitors such as coumarins are used more frequently to prevent repeated thrombosis. The basic principle during therapy is to walk and lie instead of standing and sitting. In the recent past, it has been shown that consistent compression therapy alone cannot adequately counteract the disease.
Movement is therefore an inevitable therapeutic step. In severe cases of PTS, damaged veins may need to be replaced. For this purpose, either donor veins are transplanted or vein parts are manufactured using modern technology such as the 3D printer and inserted into the patient.
Prevention
The postthrombotic syndrome can be prevented to the extent that thrombosis of the deep vein systems can be prevented. As long as there is no thrombosis, no postthrombotic syndrome can develop. In the context of thrombosis, preventive measures include, for example, a balanced diet with sufficient fluid intake and plenty of exercise. Abstinence from nicotine is also considered a preventive measure. In addition, sitting or standing for long periods of time is not recommended.
== Aftercare Almost every second patient develops a postthrombotic syndrome after deep vein thrombosis. The symptoms can then become so severe that there can be massive impairments in everyday life and the ability to work. Complete healing is hardly possible, which is why aftercare aims to improve blood circulation and reduce existing pain.
Consistent and regular follow-up treatment with follow-up examinations is therefore essential. The cornerstones of aftercare are consistent compression therapy with compression stockings (usually lifelong) and maintaining and improving the mobility of the affected patients. This is done, among other things, through adapted physiotherapy with improvement and maintenance of muscular activity in the affected areas.
This ensures a better muscle pump function. This in turn reduces congestion symptoms. In particular, the arthrogenic congestion syndrome (stiffening of the ankles) should be prevented. Just as effective and necessary is the prescription of lymphatic drainage to prevent feelings of tension and congestion symptoms.
Careful skin care should also be taken into account. The skin is more susceptible to injuries and to infectious agents, which in the worst case can lead to complications such as sepsis. Regular medical check-ups should therefore be carried out in order, as mentioned, to counteract the development of venous ulcers.
You can do that yourself
In the case of a postthrombotic syndrome (PTS), the patient should definitely become active. Because especially when the disease has not progressed too far, a lot of exercise helps the body to counteract the side effects of the syndrome. Irrespective of whether the arm or leg veins are affected, sports and types of exercise such as hiking, cycling, walking, etc. are recommended. However, overloading should be avoided.
All in all, the following rule applies to the patient: “It is better to walk and lie down than stand and sit.” However, when lying down, you should also make sure that the affected extremities are consistently elevated. At the same time, the affected areas should be compressed. This works best with support stockings and/or compression bandages. According to the doctor’s orders, they usually have to be worn at all times. Since this is often perceived as unpleasant by the patients, this therapeutic measure requires a high level of compliance. However, a compression stocking or tube not only supports the venous system, but also protects the skin from injury.
If the postthrombotic syndrome (PTS) is already advanced, the patients often suffer from water retention and joint inflammation. The inflammation can be carefully cooled by the patient himself. If you have water retention, you should see a doctor who will prescribe water-repellent agents (diuretics) if necessary.