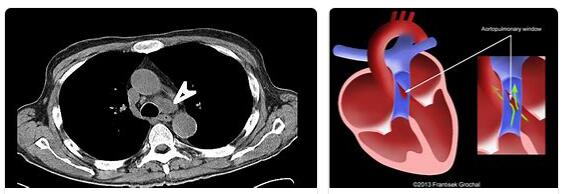
The aorto-pulmonary window is a congenital septal defect. The ascending aorta and pulmonary trunk are connected to one another within the scope of the defect and thus cause pulmonary hypertension, right-sided cardiac stress and tissue undersupply. The aorto-pulmonary septal defect is corrected by surgically separating the connected vessels.
What is an aorto-pulmonary window?
The ascending aorta and pulmonary trunk are connected to one another within the scope of the defect and thus cause pulmonary hypertension, right-sided cardiac stress and tissue undersupply.
According to electronicsmatter, the ascending aorta corresponds to the initial part of the aorta, which arises from the left ventricle. The aortic arch connects cranially to the ascending aorta. The pulmonary trunk is the trunk of the pulmonary arteries. In a healthy body there is a septal separation between this common trunk of the pulmonary arteries and the ascending aorta.
In the case of congenital malformations such as the aorto-pulmonary window, this separation is canceled. The phenomenon is a vascular malformation, also known as an aorto-pulmonary septal defect . Septal defects are incomplete occlusions of the heart septa between the left and right halves of the heart.
The blood mixes through the connection between the aorta and the pulmonary artery. The result is flooding, which usually causes damage to the lungs. Depending on the exact location and extent of the vascular defect, the doctor differentiates between four different variants of the aorto-pulmonary window.
Causes
The aorto-pulmonary window is usually caused by the patho-haemodynamic changes in the ductus arteriosus apertus. This disease is one of the congenital heart defects . Immediately after birth, there can be a physiological connection between the aorta and the pulmonary trunk, which closes in the first two days of life.
This closure is delayed or disturbed, especially in premature babies. The primary cause of the occlusive disorder is therefore likely to be an insufficient oxygen supply or a possibly increased prostaglandin level. Together with an aorto-pulmonary window, symptoms such as an interrupted aortic arch, a ventricular septal defect, an atrial septal defect, a malfunction of the right pulmonary aorta or a Fallot tetralogy occur.
More rarely, the phenomenon results from pathological changes such as a transposition of the great arteries. From a pathophysiological point of view, the faulty vascular separation in the body’s circulation results in an approximately five-fold increase in pressure compared to the pulmonary circulation. The result is a significant increase in blood flow to the pulmonary vessels.
Symptoms, ailments and signs
Patients with aorto-pulmonary septal defect suffer from consequences such as left-right shunt with pulmonary hypertension , right-sided cardiac stress and insufficient tissue supply. For this reason, pulmonary symptoms such as dyspnea or tachypnea occur. The patients therefore breathe excessively quickly or suffer from pronounced shortness of breath .
In addition, the lower respiratory tract in particular is susceptible to infection , which manifests itself in recurrent infections. Many of the patients are physically weak , appear exhausted or tire easily . Those affected often sweat faster and more extremely than the average. In some cases, people gain insufficient weight, which makes the physical weakness even worse.
The persistent left-right shunt is associated with chronic volume stress in the right heart. This additional load can result in compensatory eccentric myocardial hypertrophy , in which the tissue of the right myocardium breaks down. These breakdown symptoms lead to right heart failure . Pulmonary hypertension is also a common complication in connection with vascular malformation.
Diagnosis & course
Usually, doctors diagnose an aorto-pulmonary window immediately after birth. The affected newborns are clinically noticeable by pronounced shortness of breath and fatigue. This clinical picture prompts the doctor to initiate echocardiograms . X-ray imaging can also be performed to visualize the increased blood flow through the lung area.
On the x-ray, patients with an aorto-pulmonary window usually also show a more or less enlarged heart. As a rule, the ECG does not show any evidence of heart defects. Since the aorto-pulmonary window is in many cases only one of several vascular malformations, the cardiovascular system is examined relatively extensively after the diagnosis.
The earlier the aorto-pulmonary window is diagnosed, the better the prognosis. The correction results are mostly satisfactory. The long-term prognosis is therefore favorable for the patient.
Complications
In most cases, complications and heart problems occur through the aorto-pulmonary window. These occur mainly on the right side and can also lead to an insufficient supply of the tissue. In many cases, the patient experiences shortness of breath or shortness of breath, which can often lead to panic attacks.
The airways are often very susceptible to infections and other diseases and the person affected suffers from a general feeling of illness. As a result, everyday life is extremely restricted and physical work is usually not easily possible. Due to the symptoms in the heart, the patients suffer from heart failure and tire relatively quickly.
Because of the insufficiency, there is also increased pressure in the lungs. The disease is usually treated with surgery. If this is tackled early, there are usually no further complications or complaints. In severe cases, a lung transplant may also be necessary.
However, this only occurs if the disease was diagnosed late in adulthood. In the worst case, death can result if the transplant is unsuccessful or cannot be carried out quickly enough.
When should you go to the doctor?
The aorto-pulmonary window is one of the congenital heart defects that usually become noticeable in newborns within the first few days after birth. The aorto-pulmonary window is a short circuit between the main body artery (aorta) and the pulmonary circulation, so that the much higher systolic blood pressure peak of the body circulation is transferred to the pulmonary circulation and there causes blatant pulmonary hypertension with all the problems that develop from it.
The question of when to see a doctor is easy to answer, because an untreated aorto-pulmonary window usually has an unfavorable prognosis. Conversely, this means that surgical elimination of the short circuit between the body and pulmonary circulation as early as possible leads to a regression of the emerging secondary damage to the right heart and in the lungs. In individual cases in which the short-circuit window is less pronounced and the congenital heart defect was not noticed, the secondary damage – especially to the lungs – develops very slowly.
Cases have been reported of requiring lung transplants in adulthood. If children and adolescents show symptoms such as shortness of breath, increased breathing rate and rapid fatigue, and if there is a high susceptibility to respiratory infections, it is advisable to have the symptoms checked through a cardiologist in order to rule out the possibility of cardiac or vascular malformation that is as rapid as must be treated if possible in order to avoid irreversible damage.
Treatment & Therapy
Patients with aorto-pulmonary septal defect receive a causal treatment approach. Instead of the individual symptoms, the inadequate septal closure and thus the primary cause of the symptoms are corrected. This correction corresponds to an invasive procedure and thus takes place as part of an operation.
A heart-lung machine is usually used for this operation. This is a medical device that can replace the heart pump function and the function of the lungs for a certain period of time. During an operation with the help of the heart-lung machine, the blood leaves the body through a system of tubes, is enriched with oxygen outside the body and then returned to the body.
In principle, the surgeon separates the vessels during the operation and closes them with a patch. Depending on the severity of the existing vascular malformation, different surgical options are available. As long as the operation is performed as soon as possible after the actual diagnosis is made, excellent results can be achieved in most cases.
In rare cases, the heart defect is not diagnosed until adulthood. Because of the fixed pulmonary hypertension, no curative treatment is possible with such a late diagnosis. In this case, those affected usually receive a lung transplant .
Outlook & forecast
Aortic vascular malformation has a good prognosis if diagnosed early. Since it is diagnosed in childhood in most cases, there is a good chance of a good healing process after treatment.
The aorto-pulmonary window is corrected in a surgical procedure. The symptoms are permanently relieved and the child can be discharged as cured within a short time. In everyday life, the patient often no longer notices any impairments over the next few years.
If the malformation is only noticed in adulthood, various complaints or impairments often already exist. Although the vascular malformation in adults can also be completely corrected and cured, the patient suffers from other diseases. These sequelae have an immense impact on the patient’s recovery, which often means that it is no longer possible to be free of symptoms.
Some patients need an organ transplant to improve their health and wellbeing. The quality of life usually rises again afterwards. However, there is no complete cure. In addition, the healing process is delayed and can take several years. Often times the heart and lungs are weakened. Organ transplantation has other complications and challenges that must be overcome.
Prevention
The aorto-pulmonary window cannot be actively prevented. In any case, the disease is an extremely rare phenomenon for which there are hardly any case reports or case numbers.
Aftercare
With this disease, the person concerned is primarily dependent on a quick diagnosis with subsequent treatment in order to prevent further complications or possible cardiac death. If there is no treatment, serious complications arise that can make everyday life much more difficult for the person concerned.
Special follow-up measures are usually not available to the affected person. The earlier the disease is recognized, the better the further course will usually be. In general, with this disease, the sufferer should be mindful of a healthy lifestyle with a healthy diet. In doing so, fatty or very sweet foods should be avoided, whereby sporting activities can also have a positive effect on the course of the disease.
As a rule, however, surgical interventions are necessary. After such an operation, the person affected should rest and take care of their body. Exertion or stressful activities are not advisable, so that most patients rely on the help and care of relatives. The further course and life expectancy of the person affected depend heavily on the exact severity of the symptoms.
You can do that yourself
The peculiarity of the disease means that preventive measures have no direct influence on the course of the disease. Patients must therefore pay more attention to their general health.
The risk of recurring infections of the respiratory tract is higher than in healthy patients. Here it is important to keep a balance between overly cautious behavior that avoids real or supposed dangers (infectious environment, cold), and a slightly demanding burden on the body (stimulating climate, lightest sports such as walking in the fresh air). Regular exercise is crucial in the supportive therapy of many diseases.
Because the disease often causes shortness of breath, the aortopulmonary window can cause great anxiety and panic in the patient. Fear can be countered through targeted breathing therapy. Meditative exercises, autosuggestion and autogenic training are helpful measures for emergencies, when it is vital to suppress the panic that is emerging. Special breathing exercises are also helpful when there is an increased need for oxygen.
Patients diagnosed with an aortopulmonary window tire quickly; this must be taken into account in the environment.